Does Q1Medicare show information for sanctioned Medicare Part D and Medicare Advantage plans?
Yes. Even though Medicare plans sanctioned by the Centers for Medicare and Medicaid Services (CMS) are not allowed to accept new enrollment, Q1Medicare® shows “sanctioned” Medicare plans within the Medicare Part D Plan Finder (PDP-Finder.com) and Medicare Advantage Plan Finder (MA-Finder.com) so current plan Members can still find plan coverage information.
As an example, in September 2020, CMS sanctioned the Idaho Medicare Advantage plan “Secure Blue no Rx (PPO) - H1302-004-0 and prohibited the Medicare Advantage plan from accepting plan enrollments "beginning January 1, 2021, through December 1, 2021". However, current plan members were not affected by the CMS sanctions and were allowed to remain with the Medicare plan into 2021 - and still would need information about their 2021 Medicare plan coverage.
To provide information about this example 2021 Medicare plan, we displayed the “Secure Blue no Rx (PPO) - H1302-004-0” within our Medicare Advantage Plan Finder marked with a dark red rectangle and the text “Sanctioned Plan” (see: MA-Finder.com/2021/83713).
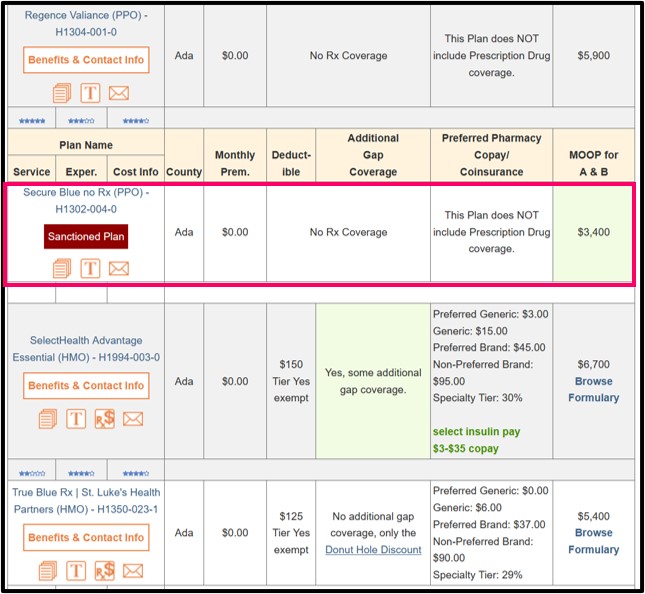
If a person wishes to see more coverage information, they can click on the Medicare Advantage plan's name or the “Sanctioned Plan” button and they will be shown the plan benefit details along with another large dark red box with the message: "This Plan is currently sanctioned and is not accepting enrollments".
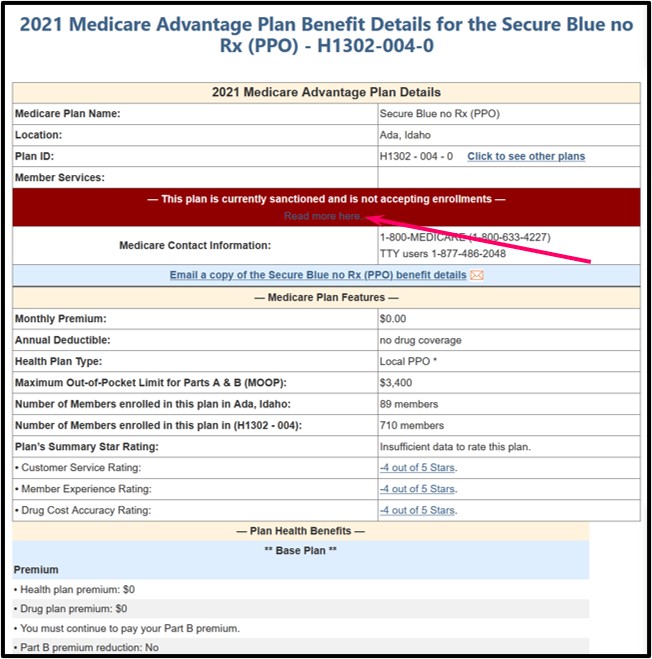
Within the dark red rectangle on the plan details page, the user is also provided with a link to the Q1Medicare news article about the actual CMS sanction, in this case: “CMS Notice of Enrollment Suspension for Medicare Advantage-Prescription Drug Contract Number H1302 (Blue Cross of Idaho Care Plus, Inc.) for plan year 2021” (please see: Q1News.com/849).
The Q1News article also provides a link to the actual CMS letter that was sent to the plan.

The Medicare.gov Plan Finder also provides sanctioned plan information after you click on the "View sanctioned plans" link found at the bottom of the plan summary page. However, as of April 29, 2021, Medicare only shows basic plan contact information and a link to the sanctions letter from CMS. Plan coverage information for current members of the sanctioned Medicare plan is not provided.
As an example, in September 2020, CMS sanctioned the Idaho Medicare Advantage plan “Secure Blue no Rx (PPO) - H1302-004-0 and prohibited the Medicare Advantage plan from accepting plan enrollments "beginning January 1, 2021, through December 1, 2021". However, current plan members were not affected by the CMS sanctions and were allowed to remain with the Medicare plan into 2021 - and still would need information about their 2021 Medicare plan coverage.
To provide information about this example 2021 Medicare plan, we displayed the “Secure Blue no Rx (PPO) - H1302-004-0” within our Medicare Advantage Plan Finder marked with a dark red rectangle and the text “Sanctioned Plan” (see: MA-Finder.com/2021/83713).

If a person wishes to see more coverage information, they can click on the Medicare Advantage plan's name or the “Sanctioned Plan” button and they will be shown the plan benefit details along with another large dark red box with the message: "This Plan is currently sanctioned and is not accepting enrollments".

Within the dark red rectangle on the plan details page, the user is also provided with a link to the Q1Medicare news article about the actual CMS sanction, in this case: “CMS Notice of Enrollment Suspension for Medicare Advantage-Prescription Drug Contract Number H1302 (Blue Cross of Idaho Care Plus, Inc.) for plan year 2021” (please see: Q1News.com/849).
The Q1News article also provides a link to the actual CMS letter that was sent to the plan.

The Medicare.gov Plan Finder also provides sanctioned plan information after you click on the "View sanctioned plans" link found at the bottom of the plan summary page. However, as of April 29, 2021, Medicare only shows basic plan contact information and a link to the sanctions letter from CMS. Plan coverage information for current members of the sanctioned Medicare plan is not provided.
Reminder about Special Enrollment Period (SEP) that may be available to members of sanctioned Medicare plans.
A case-by-case SEP is available to members of a sanctioned Medicare plan if they can show that they were affected by plan practices that were at issue in the sanction. To learn more, please speak with a Medicare representative (1-800-633-4227). Again, this SEP is not automatically granted and is considered on a case-by-case basis.
Sources include:
CMS, "Notice of Enrollment Suspension for Medicare Advantage-Prescription Drug Contract Number H1302", September 9, 2020,
https://www.cms.gov/files/document/blue-cross-idaho-care-plus-inc.pdf
Browse FAQ Categories
Pets are Family Too!
Use your drug discount card to save on medications for the entire family ‐ including your pets.
- No enrollment fee and no limits on usage
- Everyone in your household can use the same card, including your pets
Your drug discount card is available to you at no cost.
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
