What happens when a person is "crosswalked" to another Medicare Part D plan?
The term "crosswalked" refers to how a Medicare beneficiary is automatically transferred or moved from one Medicare plan to another Medicare Part D plan or Medicare Advantage plan for the following year - crosswalks can be part of Medicare plan mergers or consolidations or being splitting apart based into small pieces or changes in Contract ID/Plan IDs.
For example, you are enrolled in the 2023Medicare plan "ABC" and your plan mergers with Medicare plan "XYZ", in 2024, you will be automatically moved from your ABC plan to the new 2024 Medicare plan XYZ - however, you still have the option of choosing a different 2024 Medicare plan on your own -- during the Annual Enrollment Period (AEP).
Important: If you are crosswalked into another Medicare plan, your plan coverage may not be the same as your original plan.
Please remember that a Medicare plan can also change names year-to-year - with new coverage features (premium, deductibles, co-pays).
Usually, you will learn of the transfer to another Medicare plan when you receive your Annual Notice of Change (ANOC) letter from your current Medicare Part D prescription drug plan or Medicare Advantage plan.
If you are crosswalked or transferred to another Medicare plan, your new plan will be effective starting in the next plan year (January 1), along with any coverage changes that the new plan provides - unless you choose to enroll in another Medicare Part D or Medicare Advantage plan during the annual Open Enrollment Period (AEP) that starts on October 15th and continues through December 7th, with your new Medicare plan coverage beginning on January 1st. To change your Medicare plan coverage outside of the AEP, you must qualify for a Special Enrollment Period.
Need a way to see if your Medicare Part D or Medicare Advantage plan is changing next year?
Our PDP-Compare and MA-Compare tools allow you to compare annual changes in all stand-alone Medicare Part D prescription drug plans (PDPs) or Medicare Advantage plans (MAs or MAPDs) across the country showing changes in monthly premiums and plan design changes, as well as changes in co-payments or co-insurance rates for different drug tiers along with the most recent Medicare Star ratings.
Both the PDP-Compare and MA-Compare also show the Medicare Part D plans or Medicare Advantage plans that will be merged, discontinued, or added next year.
Since 2006, Medicare plan mergers and consolidations have become a normal occurrence and each year, a number of people are crosswalked or automatically transferred into other Medicare plans.
For example, you are enrolled in the 2023Medicare plan "ABC" and your plan mergers with Medicare plan "XYZ", in 2024, you will be automatically moved from your ABC plan to the new 2024 Medicare plan XYZ - however, you still have the option of choosing a different 2024 Medicare plan on your own -- during the Annual Enrollment Period (AEP).
Important: If you are crosswalked into another Medicare plan, your plan coverage may not be the same as your original plan.
Please remember that a Medicare plan can also change names year-to-year - with new coverage features (premium, deductibles, co-pays).
Usually, you will learn of the transfer to another Medicare plan when you receive your Annual Notice of Change (ANOC) letter from your current Medicare Part D prescription drug plan or Medicare Advantage plan.
If you are crosswalked or transferred to another Medicare plan, your new plan will be effective starting in the next plan year (January 1), along with any coverage changes that the new plan provides - unless you choose to enroll in another Medicare Part D or Medicare Advantage plan during the annual Open Enrollment Period (AEP) that starts on October 15th and continues through December 7th, with your new Medicare plan coverage beginning on January 1st. To change your Medicare plan coverage outside of the AEP, you must qualify for a Special Enrollment Period.
Need a way to see if your Medicare Part D or Medicare Advantage plan is changing next year?
Our PDP-Compare and MA-Compare tools allow you to compare annual changes in all stand-alone Medicare Part D prescription drug plans (PDPs) or Medicare Advantage plans (MAs or MAPDs) across the country showing changes in monthly premiums and plan design changes, as well as changes in co-payments or co-insurance rates for different drug tiers along with the most recent Medicare Star ratings.

Both the PDP-Compare and MA-Compare also show the Medicare Part D plans or Medicare Advantage plans that will be merged, discontinued, or added next year.
Since 2006, Medicare plan mergers and consolidations have become a normal occurrence and each year, a number of people are crosswalked or automatically transferred into other Medicare plans.

Examples of Annual Medicare plan Crosswalks
- 2023 Medicare plan members crosswalked to new 2024 plans:
Over 2.7 million people – 2.6 million
enrolled in 2023 Medicare Advantage plans and an additional 118,000 people
enrolled in 2023 stand-alone Medicare Part D plans – will be automatically
“crosswalked” or merged into a different 2024 Medicare plan.
For example, members of the 2023 Clear Spring Health Premier Rx (PDP) will be automatically reassigned to the 2024 Clear Spring Health Value Rx (PDP).
- 2022 Medicare plan members crosswalked to new 2023 plans: Almost 1.5 million people – 1.47 million enrolled in 2022 Medicare Advantage plans and an additional 200,000 people enrolled in 2022 stand-alone Medicare Part D plans – will be automatically “crosswalked” or merged into a different 2023 Medicare plan. For example, members of the 2022 Cigna Essential Rx (PDP) will be automatically reassigned to the 2023 Cigna Extra Rx (PDP). You can click here to read more about Medicare plan mergers or consolidations.
- 2021 Medicare plan members crosswalked to new 2022 plans: Over 4.4 million people – 3.2 million people enrolled in 2021 stand-alone Medicare Part D plans and an additional 1.2 million enrolled in 2021 Medicare Advantage plans – will be automatically “crosswalked” or merged into a different 2022 Medicare plan. For example, members of the 2021 Florida Wellcare Rx (PDP) will be automatically reassigned to the 2022 Wellcare Value Script (PDP). You can click here to read more about Medicare plan mergers or consolidations.
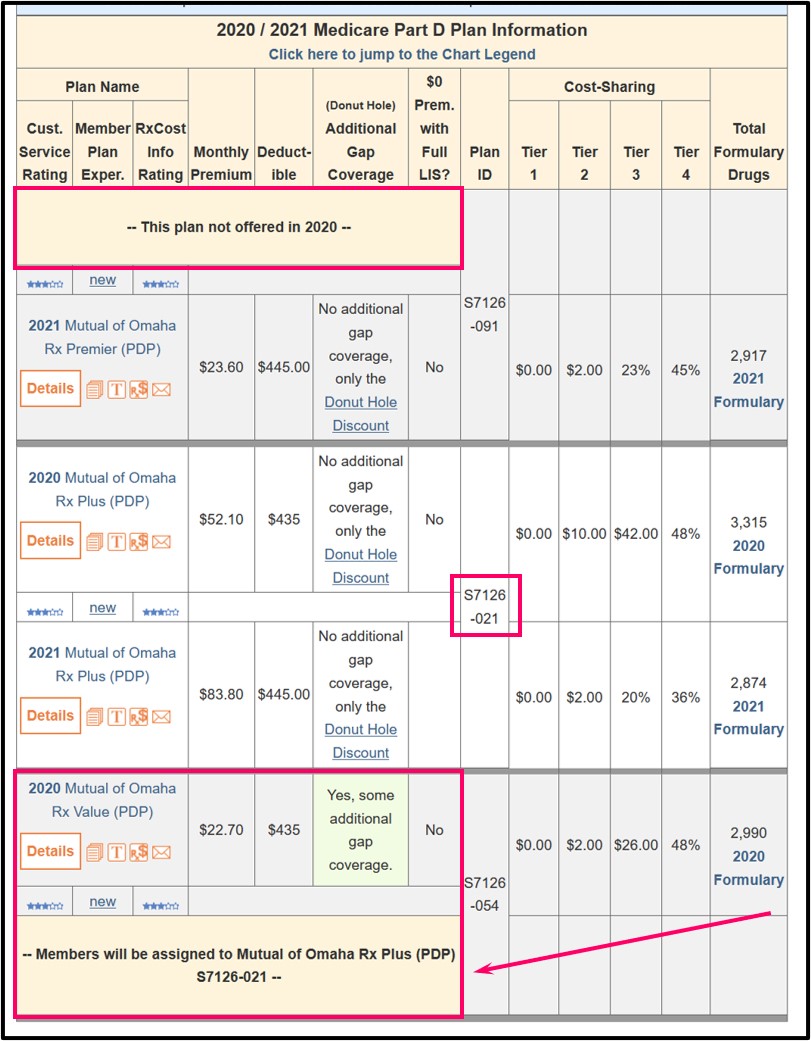
- 2020 Medicare plan members crosswalked to new 2021 plans: Over 1.3 million people enrolled in 2020 Medicare Advantage plan and an additional 187,000 people enrolled in a 2020 stand-alone Medicare Part D plan will be automatically “crosswalked” or merged into another 2021 Medicare plan. For example, members of the 2020 Texas Mutual of Omaha Rx Value (PDP) will be automatically reassigned to the 2021 Mutual of Omaha Rx Plus (PDP). You can click here to read more about 2020/2021 Medicare plan mergers or consolidations.
- 2019 members crosswalked to new 2020 plans: Approximately 744,400 members in non-renewing 2019 stand-alone Medicare
prescription drug plans (PDPs) and an additional 2,069,600 members in
non-renewing Medicare Advantage plans (MA and MAPDs) were
automatically "crosswalked" to new 2020 Medicare plans. For example,
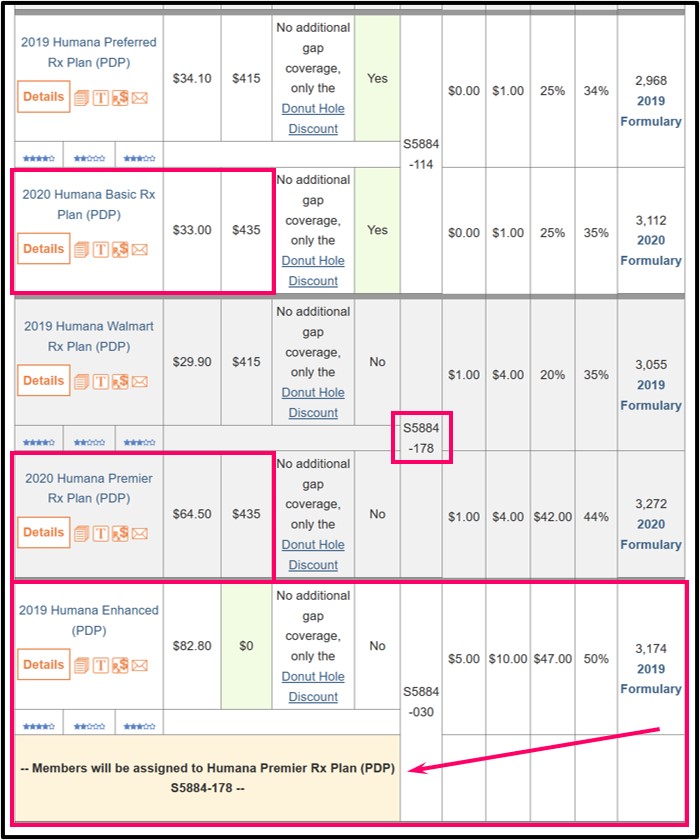
members of the 2019 Humana Enhanced (PDP) Medicare Part D plan were automatically reassigned to the 2020 Humana Premier Rx Plan (PDP). You can click here to read more about 2020 Medicare Part D plan mergers or consolidations. You can see the transition on our Medicare Part D
2019/2020 Compare page:
PDP-Compare.com/CA
- 2018 members crosswalked to new 2019 plans: Over 800,000 current members of stand-alone 2018 Medicare Part D plans
and 200,000 Medicare Advantage plan members were automatically
“crosswalked” or merged into another Medicare plan in 2019. For example,
members of the 2018 Symphonix Value Rx (PDP) were automatically reassigned to the 2019 AARP MedicareRx Saver Plus (PDP). You can click here to read more about 2019 Medicare Part D plan mergers or consolidations.
- 2017 members crosswalked to new 2018 plans: Over 200,000 current members of stand-alone 2017 Medicare Part D
plans and Medicare Advantage plans were automatically “crosswalked”
or merged into another Medicare plan in 2018. For example, members of
the 2017 First Health Part D Premier Medicare Part D plan (PDP) were automatically
reassigned to the 2018 First Health Part D Value Plus (PDP). You can click here to read more about 2018 Medicare Part D plan mergers or consolidations.
- 2016 members crosswalked to new 2017 plans: In 2016, the California WellCare Classic and WellCare Extra were still being offered
in 2017, however, the Contract ID / Plan ID changed moving the plan members:
2016 WellCare Extra (PDP) - S5967-203
2017 WellCare Extra (PDP) - S4802-128 and
2016 WellCare Classic (PDP) - S5967-169
2017 WellCare Classic (PDP) - S4802-094
You can click here to read more about the 2016/2017 Medicare Part D plan mergers or consolidations.
- 2015 members crosswalked to new 2016 plans: In 2015, approximately 260,000 members of stand-alone Medicare Part D plans were “crosswalked” or merged into another Medicare Part D plan in 2016. As an example, members of the 2015 SmartD Rx Saver (PDP) were automatically reassigned to the 2016 Express Scripts Medicare - Value (PDP). You can click here to read more about the 2016 Medicare Part D plan mergers or consolidations.
Browse FAQ Categories
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
