Can I see the history of Medicare Part D retail drug prices or how drug prices have changed over time?
Yes. We show the
average negotiated retail drug price in the far right column of our Q1Rx.com Drug
Finder comparison chart - and when you click on the retail price we show more information about drug costs - including the historical retail prices.
Remember: We show the average negotiated retail drug prices - and you will find that the actual retail prices can vary pharmacy-to-pharmacy (so CVS retail prices may not be the same as prices at WalMart or Walgreens) and prices can change week-to-week. Also, please note that the average negotiated retail drug price can vary state-to-state as you travel with your Medicare Part D plan.
Here is an example of our Q1Rx.com Drug Finder showing how the retail price of a popular generic medication can vary between Medicare Part D plans (the estimated cost using a Drug Discount Card is shown at the top of the Q1Rx table).
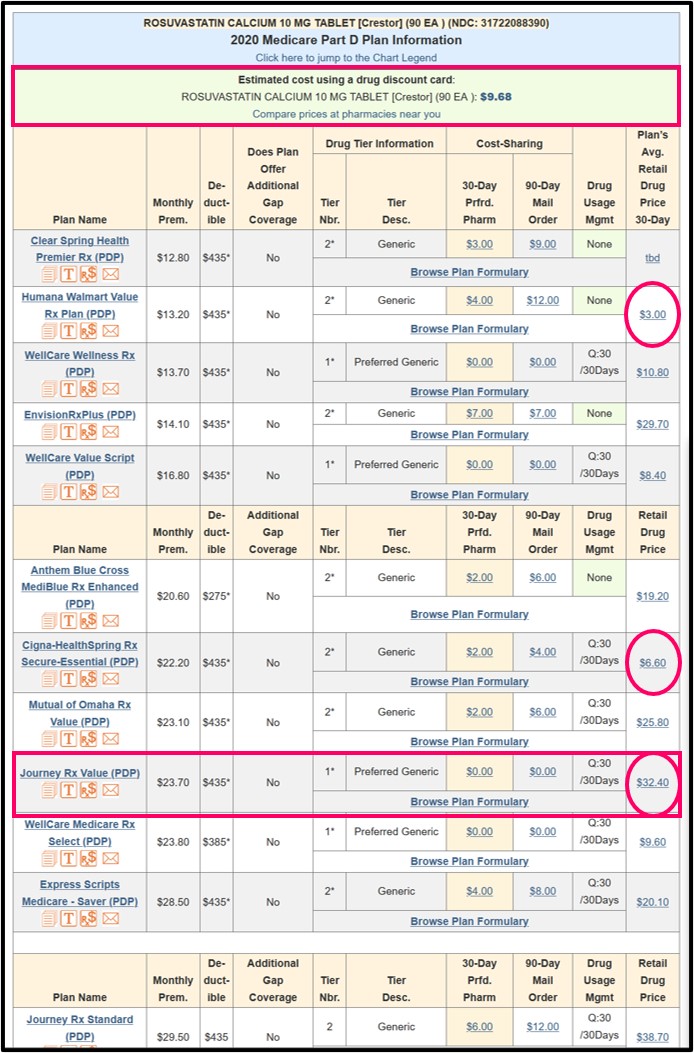
Remember: We show the average negotiated retail drug prices - and you will find that the actual retail prices can vary pharmacy-to-pharmacy (so CVS retail prices may not be the same as prices at WalMart or Walgreens) and prices can change week-to-week. Also, please note that the average negotiated retail drug price can vary state-to-state as you travel with your Medicare Part D plan.
Here is an example of our Q1Rx.com Drug Finder showing how the retail price of a popular generic medication can vary between Medicare Part D plans (the estimated cost using a Drug Discount Card is shown at the top of the Q1Rx table).

Seeing how retail drug prices can change over time.
To see how a retail price can change with a certain Medicare Part D plan, you can click on the average negotiated retail drug price (in this example, the Cigna-HealthSpring price of $6.60) to view the pricing history for a particular plan and drug.
The same average retail drug pricing information is also available when using our Formulary Browser and clicking on the 30-day supply or 90-day supply cost-sharing figures.
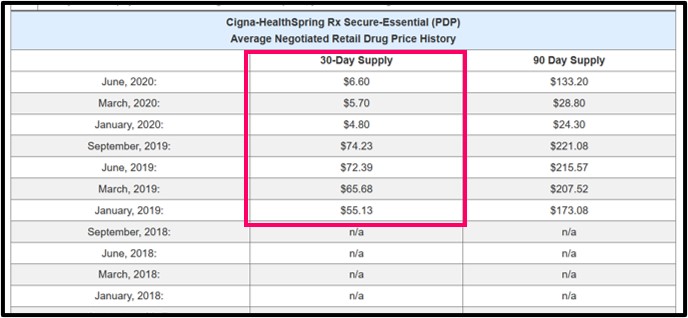
See the 2021 Rosuvastatin data and see the current Rosuvastatin data.
Question: Why are retail drug prices important when you have Medicare drug coverage?
Higher retail drug costs can mean that you pay more for your drug coverage - and higher retail drug prices mean that you move faster through the phases of your Medicare drug coverage.
See the 2021 Rosuvastatin data and see the current Rosuvastatin data.
Higher retail drug costs can mean that you pay more for your drug coverage - and higher retail drug prices mean that you move faster through the phases of your Medicare drug coverage.
- Retail drug costs determine the time you spend in the Initial Deductible.
If your Medicare prescription drug plan has an initial deductible, retail drug prices will affect how long you stay in the
deductible.
- Retail drug costs determine the time you spend in the Initial Coverage Phase before reaching the Coverage Gap.
You receive initial coverage until you reach your plan's Initial Coverage Limit (ICL) and your plan's negotiated retail cost for your medication is used to determined when you reach your ICL. For example, if you purchase a medication with a retail cost of $500 and you have a co-pay of $60, the $500 retail value is counted toward meeting your Initial Coverage Limit - and when you exceed the Initial Coverage Limit, you enter the Coverage Gap or Donut Hole - and pay 75% of the plan's retail price.
- Retail drug costs can determine what you will pay in the Initial Coverage phase.
If your Medicare prescription drug plan uses co-insurance cost sharing, then you will pay a percentage of the retail drug costs for your formulary drugs. For example, if you pay a 25% co-insurance for a medication that has a negotiated retail drug price of $100, your cost-sharing is $25 - and the $100 retail cost is counted toward the Initial Coverage Limit. If the retail drug price increases to $200 during the plan year, you will pay $50 for the same medication - even though the coverage cost was $25 for the same drug back when you enrolled in the plan.
- Retail drug costs dictate what you pay in the Donut Hole.
Once you are in the Donut Hole or Coverage Gap, you will receive the 75% Donut Hole discount for all formulary drugs. In other words, you pay 25% of the retail cost for your formulary prescriptions.
- Retail drug prices determine what you pay in the Catastrophic Coverage phase.
If you have high out-of-pocket spending, you may enter the Catastrophic Coverage phase and your cost-sharing while in the Catastrophic Coverage phase (after leaving the Donut Hole) can vary depending on the retail price of your drugs. For example, in 2021, you pay the greater of $3.70 or 5% of your plan’s negotiated retail drug price for generics or the higher of $9.20 or 5% of the retail cost of your brand-name drugs.
See the 2021 Rosuvastatin data and see the current Rosuvastatin data.
Browse FAQ Categories
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
