What should I do if my Medicare Part D drug plan no longer covers one of my expensive medications?
If one of your medications is no longer covered by your Medicare Part D prescription drug plan, there are at least three steps you can take at this time:
(1) If your medication is not excluded from the Medicare program, you can ask your Medicare prescription drug plan for a one-time, transition fill or temporary supply of your medication for 30 days. You can click here to read more about transition fills.
(2) While you are using your 30-day temporary medication supply (transition fill), you and your physician can look for a generic equivalent or an alternative medication that is included on your Part D plan’s formulary.
Tip: See the information below about our Formulary Browser and to learn more about reviewing your plan’s drug list online.
(3) If you cannot find an alternative medication on your plan's formulary, you can file a formulary exception request with your Medicare Part D plan asking that your non-formulary medication be covered under your current Medicare plan. Click here to learn more about requesting a formulary exception or you can click here to learn about the prescribing physician’s role in the formulary request process.
Important reminder: Remember that your transition fill is only for a 30-day supply, so start working with your prescriber right away to find an alternative medication or file a formulary exception request.
Also, formulary exception requests are not “automatically” granted.
If your formulary exception request is denied, you have the right to appeal your plan’s decision a number of times, ultimately with a review by an independent group. You can click here for an overview of the appeals process.
(1) If your medication is not excluded from the Medicare program, you can ask your Medicare prescription drug plan for a one-time, transition fill or temporary supply of your medication for 30 days. You can click here to read more about transition fills.
(2) While you are using your 30-day temporary medication supply (transition fill), you and your physician can look for a generic equivalent or an alternative medication that is included on your Part D plan’s formulary.
Tip: See the information below about our Formulary Browser and to learn more about reviewing your plan’s drug list online.
(3) If you cannot find an alternative medication on your plan's formulary, you can file a formulary exception request with your Medicare Part D plan asking that your non-formulary medication be covered under your current Medicare plan. Click here to learn more about requesting a formulary exception or you can click here to learn about the prescribing physician’s role in the formulary request process.
Important reminder: Remember that your transition fill is only for a 30-day supply, so start working with your prescriber right away to find an alternative medication or file a formulary exception request.
Also, formulary exception requests are not “automatically” granted.
If your formulary exception request is denied, you have the right to appeal your plan’s decision a number of times, ultimately with a review by an independent group. You can click here for an overview of the appeals process.
Question: Is there a quick way for me to see the medications covered by my Medicare prescription drug plan?
Yes. We have an online Formulary Browser that lets you browse through any Medicare Part D (PDP) or Medicare Advantage (MAPD) plan drug list.
1. To begin, you can click here or go to FormularyBrowser.com.
2. Select either PDP (drug only plans) or MAPD (health and drug plans), then choose your state, the name of your Medicare plan provider (such as AARP or Humana), and click “Search”.
3. Next, choose the specific name of your Medicare plan as offered by your provider (such as the AARP MedicareRx Preferred plan), and click “Search” again.
You can then browse alphabetically through the plan’s entire formulary (the letter “A” is chosen by default).
Please notice that in the search box, you see the formulary drug tiers and the number of drugs on each tier, and you can hide tiers from the results, for example, if you only want to see Tier 1 drugs.
The results will show you the medication name, the drug tier, the cost-sharing at a preferred network pharmacy, and any drug utilization management restrictions.
You can click on the 30- or 90-day cost-sharing figures (such as $10.00 for Tier 1 drugs in Florida) to see additional pricing details and the average retail cost history.
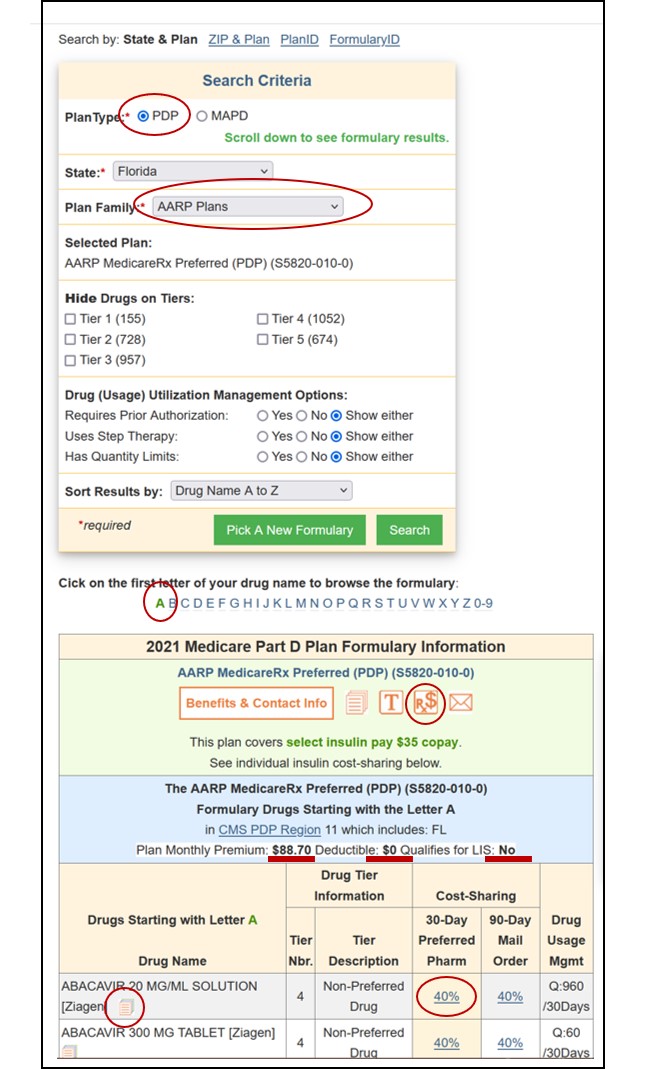
Reminder: Both our Formulary Browser (showing all drugs for a single Medicare plan) and our Drug Finder (showing all Medicare plans covering a single drug) display the drug cost-sharing information, along with the details of the drug utilization management restrictions (for example, Q: 30/30Days for a quantity limit) for all Medicare Part D plans and Medicare Advantage plans.
Tip: If you are browsing plans using our Medicare Part D or Medicare Advantage plan search tools (PDP-Finder.com or MA-Finder.com), the right-hand column of the results chart, shows a “Browse Formulary” link taking you directly to your chosen plan’s online formulary.
News Categories
Pets are Family Too!
Use your drug discount card to save on medications for the entire family ‐ including your pets.
- No enrollment fee and no limits on usage
- Everyone in your household can use the same card, including your pets
Your drug discount card is available to you at no cost.
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
