What is Medicare prescription drug coverage?
Medicare prescription drug coverage is insurance for a specific list of out-patient prescription drugs and you use your drug coverage like any other types of insurance:
(1) You may pay a monthly premium for the drug coverage.
You usually pay a monthly premium for stand-alone Medicare Part D drug coverage from around $12 to $190. However, you can also receive Medicare drug coverage if you enroll in a Medicare Advantage plan that has drug coverage - and your premium may be $0.
(2) Your drug plan may have an Initial Deductible where you pay 100% before coverage starts.
You may pay an initial deductible where you are 100% responsible for your drug costs before you and your drug plan begin to share the cost of drug coverage - although some drug plans have a $0 deductible - and many drug plans have an initial deductible but will exclude low-costing generics from the deductible.
(3) After the Initial deductible (if any), you will sharing the cost of drug coverage with your plan.
Once you are through your deductible (if any), you and your insurance share a portion of the coverage costs for formulary drugs (for example, your plan pays 75% of retail drug prices and you pay the 25% balance (so you would pay $25 for a $100 drug) - or you pay a $2 co-pay for your generic drugs (so you may pay $2 for a $15 generic).
(4) You drug coverage is limited to the drugs on your plan's drug list (or drug formulary)
Your Medicare Part D plan (drug insurance) will not cover all medications and you need to be sure that you choose a drug plan with a formulary (drug list) that includes your prescriptions - with the knowledge that a formulary can change throughout the plan year (usually substituting newly-released generic drugs for higher-costing brand-name drugs).
(5) You must be eligible to join a Medicare drug plans
Medicare prescription drug coverage is available to everyone with Medicare Part A and/or Medicare Part B coverage - who reside in the Medicare plan's Service Area (state, county, or ZIP code). A Medicare Advantage plan (with or without drug coverage) requires you to have both Medicare Part A and Part B.
(1) You may pay a monthly premium for the drug coverage.
You usually pay a monthly premium for stand-alone Medicare Part D drug coverage from around $12 to $190. However, you can also receive Medicare drug coverage if you enroll in a Medicare Advantage plan that has drug coverage - and your premium may be $0.
(2) Your drug plan may have an Initial Deductible where you pay 100% before coverage starts.
You may pay an initial deductible where you are 100% responsible for your drug costs before you and your drug plan begin to share the cost of drug coverage - although some drug plans have a $0 deductible - and many drug plans have an initial deductible but will exclude low-costing generics from the deductible.
(3) After the Initial deductible (if any), you will sharing the cost of drug coverage with your plan.
Once you are through your deductible (if any), you and your insurance share a portion of the coverage costs for formulary drugs (for example, your plan pays 75% of retail drug prices and you pay the 25% balance (so you would pay $25 for a $100 drug) - or you pay a $2 co-pay for your generic drugs (so you may pay $2 for a $15 generic).
(4) You drug coverage is limited to the drugs on your plan's drug list (or drug formulary)
Your Medicare Part D plan (drug insurance) will not cover all medications and you need to be sure that you choose a drug plan with a formulary (drug list) that includes your prescriptions - with the knowledge that a formulary can change throughout the plan year (usually substituting newly-released generic drugs for higher-costing brand-name drugs).
(5) You must be eligible to join a Medicare drug plans
Medicare prescription drug coverage is available to everyone with Medicare Part A and/or Medicare Part B coverage - who reside in the Medicare plan's Service Area (state, county, or ZIP code). A Medicare Advantage plan (with or without drug coverage) requires you to have both Medicare Part A and Part B.
Question: What are the different ways to get Medicare Part D prescription drug coverage?
Medicare drug plans are provided by private companies that have been approved by the Centers for Medicare & Medicaid Services (CMS or Medicare). Your Medicare Part D prescription drug coverage can be provided by:
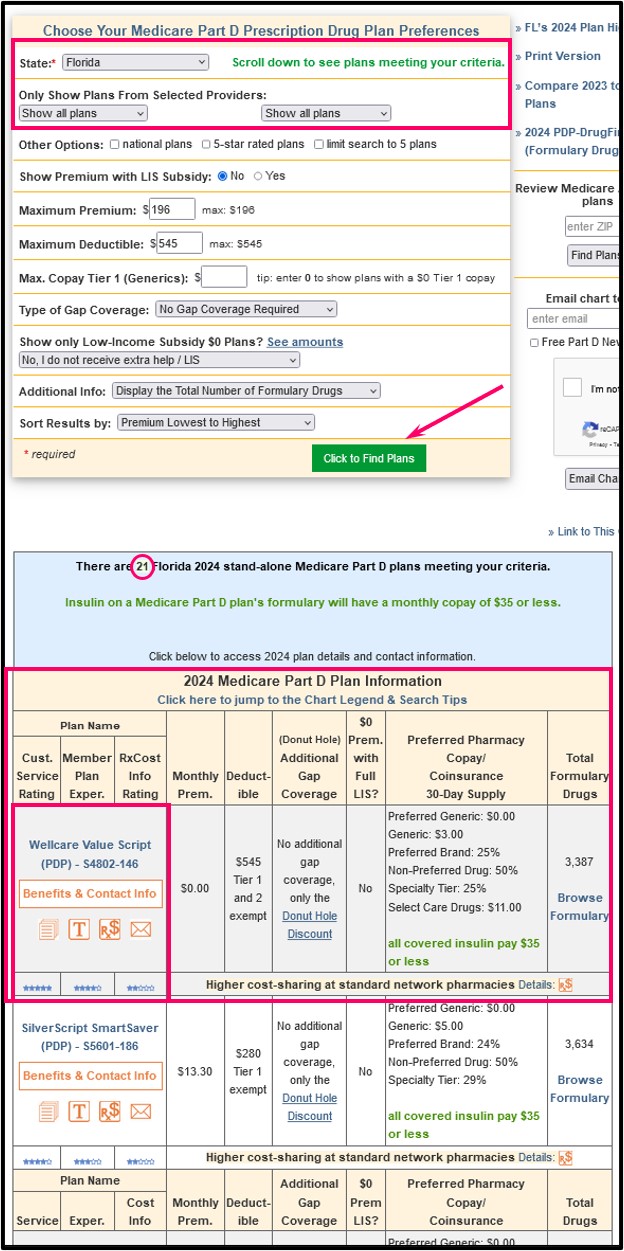
- A "stand-alone" Medicare Part D prescription drug plan (PDP)
A PDP only provides prescription coverage and usually no additional benefits. You can use our Medicare Part D Plan Finder to review all Medicare Part D plans available in your state: PDP-Finder.com.
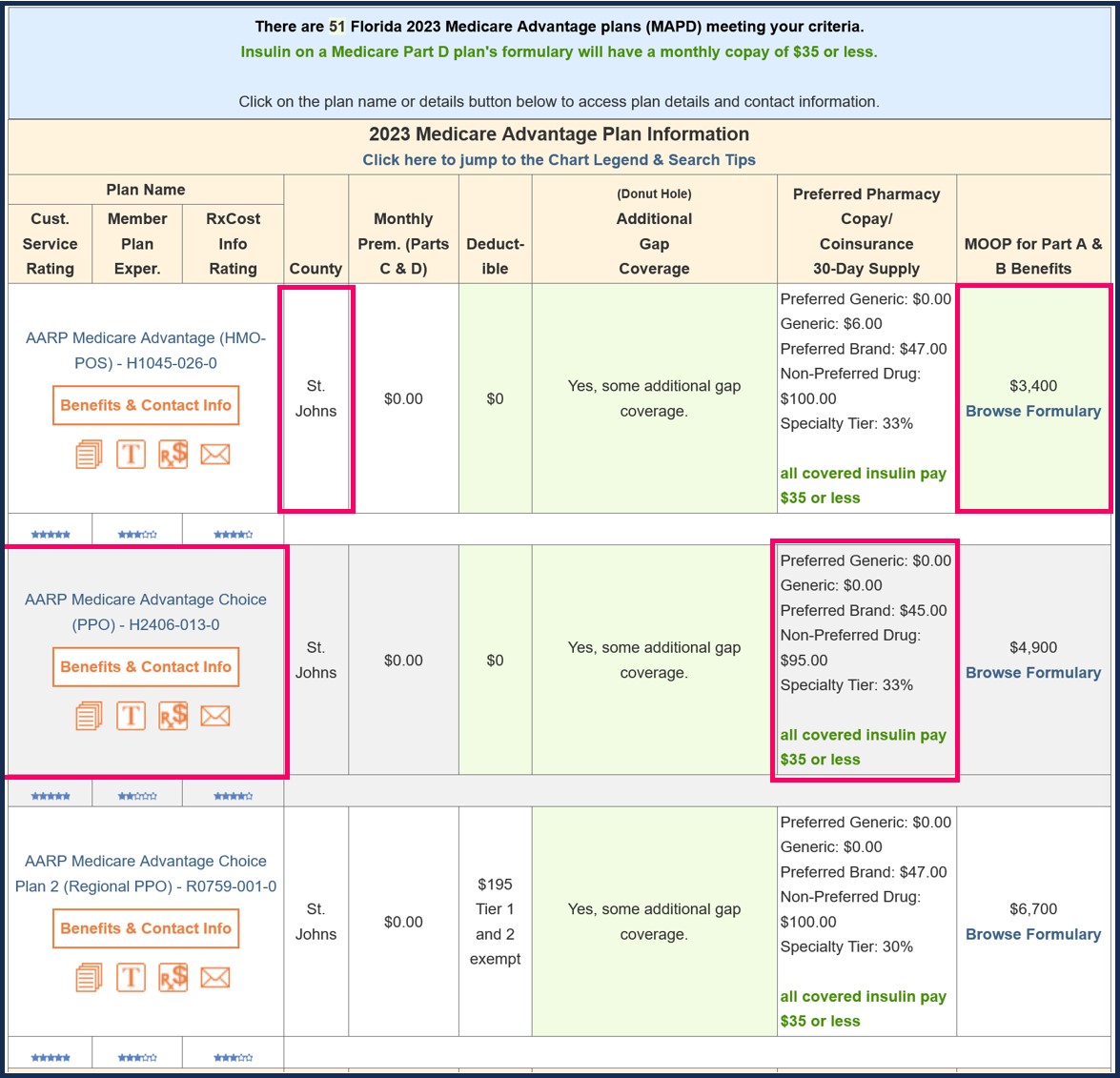
- A Medicare Advantage plan that includes prescription coverage (MAPD)
An MAPD includes your Medicare Part D prescription drug coverage - plus includes Medicare Part A coverage (for in-patient and hospital care) - plus Medicare Part B coverage (for out-patient and physician care) - and often other benefits such as basic dental coverage, optical coverage, hearing aid coverage, and fitness coverage (maybe even transportation coverage, home healthcare, and other supplemental benefits) - all for one monthly premium. Medicare Advantage plans are also called Medicare Part C. You can use our Medicare Advantage Plan Finder tool to see all Medicare Advantage plans available in your county: MA-Finder.com. - Finally, you can also receive prescription drug coverage from other sources such as your Union, Employer Health Plan, TRICARE for Life, or the Veterans Affairs (VA).
Question: If I have employer drug coverage can I also join a Medicare Part D drug plan?
Probably not. Warning: If you have an employer health plan that includes prescription drug coverage - and then enroll in a Medicare Part D plan, you risk losing all of your employer health plan coverage, not just drug coverage. You can learn more in our employer health plan FAQs about checking with your plan administrator before enrolling in a Medicare prescription drug plan.
Question: If I have drug coverage through the Veterans Affairs (VA) can I join a Medicare Part D plan?
Yes. If you have VA coverage (that is, prescription drug coverage as part of Veterans Affairs benefits), then you may not need Medicare Part D coverage. However, if you find that the VA does not cover all of your medication needs, you can also enroll in a Medicare Part D program. The two programs cannot be used at the same time for the purchase of a single drug, but actually work together, allowing coordinated coverage - first under the VA and secondly under your Medicare Part D plan. Your VA coverage is also considered "creditable coverage" and should you decide to enroll into such a Medicare Part D plan after the close of your initial enrollment period, there will be no penalty for late enrollment. You can learn more in our VA and TRICARE FAQs.
Question: Are all Medicare Part D plans about the same and available everywhere?
No. Medicare Part D coverage will vary plan-to-plan and not all Medicare plans are available in all areas of the country. Remember: Medicare Part D and Medicare Advantage plans are offered in specific Service Areas, such as multiple-states, counties, ZIP code areas, or parts of a highly-populated city such as New York or Los Angeles. This means: If you live in Saint Johns County, Florida, you will not have the same selection of Medicare plans as your friends who live in Orange County, California. Our Q1Medicare.com tools are designed to provide people with an overview of all Medicare plan options in their area or region. For more information on Medicare prescription drug coverage, please call Medicare at 1-800-633-4227.
Question: When can I enroll into a Medicare Part D plan?
Your Initial Enrollment Period - If you are new to Medicare, you have an Initial Enrollment Period (IEP) that is a seven (7) month window beginning three (3) months before your month of eligibility, plus the month of eligibility, and ends three (3) months after your month of eligibility. If you enroll in the three months prior to your month of Medicare eligibility, your effective date (when your plan coverage begins) is the 1st day of your month of Medicare eligibility. If you enroll into a Medicare Part D plan during your month of eligibility (such as when you turn 65) or during the three months following the month of Medicare eligibility, your Medicare Part D plan will be effective on the 1st day of the month following receipt of your plan enrollment.
The annual Open Enrollment Period - If you are already eligible for Medicare, you can change Medicare plans during the Annual Enrollment Period (AEP). The Annual Enrollment Period starts each year on October 15th and continues through December 7th with your Medicare Part D plan becoming effective on January 1st of the new plan year. This time period can also be called the annual Open Enrollment Period -- which is still referred to as "AEP".
Special Enrollment Periods - If you are outside of your IEP or AEP, then you will need to use a Special Enrollment Period (SEP) to change Medicare Part D or Medicare Advantage plans. An SEP may be granted when you move outside of your plan's Service Area (move to another state) or move into an assisted living facility or when you qualify for Extra Help. If you are entitled to an SEP, your Medicare Part D plan will become effective on 1st day of the month following the receipt of your enrollment. See our Special Enrollment Period FAQ for more details and examples of SEPs.
Question: Can you join a Medicare drug plan even though you have outstanding health issues?
Yes. There are no medical limitations to joining a Medicare Part D plan and since 2021, there are no medical limitations when enrolling in a Medicare Advantage plan that provides prescription drug coverage (MAPD). From 2006 to 2020, Medicare Advantage plans required that the Member did do not suffer from End Stage Renal Disease (ESRD) or (kidney failure).
You can choose and join any Medicare drug plan that works for you and is available in your area.
Question: How much will I pay per month for a drug plan?
You will have to pay a monthly premium like you would for other insurance and premiums can range to $0 (for a MAPD plan) up to over $100 per month. If you qualify for the Medicare Part D financial Extra Help program (or Low-Income Subsidy) and enroll in a Medicare Part D plan that meets your state's $0 low-income subsidy benchmark your monthly premium will be $0.
All drug plans must provide coverage that is at least as good as standard Medicare prescription drug coverage. Some plans might offer more coverage and additional drugs for higher monthly premiums.
Question: Am I required to join a Medicare Part D plan?
No. The Medicare Part D program is voluntary and you are not required to enroll into a Medicare Part D plan when you first become eligible for Medicare. However, if you do not have some other form of creditable prescription drug coverage and then later decide to join a Part D plan (PDP or MAPD) you may incur a permanent late-enrollment penalty that you will pay in addition to your monthly plan premiums.
Question: If I don't join a drug plan when I am first eligible, how is the Late-Enrollment Penalty calculated?
Late-Enrollment Penalties are assessed when you eligible for Medicare Part D coverage, but are without some form of creditable drug coverage for more than 63 days. You can learn more in our late-enrollment premium penalty FAQs. Late-enrollment penalties are permanent and can change (increase) year-to-year. You will pay 1% of the national base Medicare Part D premium (about $33) for every month that you were without some creditable prescription drug coverage before you enrolled in a Medicare Part D plan. So, if you were eligible for Medicare when you were 65 and now you are 70, you would pay 60 months worth of penalty (5 years * 12) or about 60% of the annual base premium (so around $33 * .6 = $20 per month in addition to your monthly Part D plan premium).
Question: Is there financial assistance to help me pay my Medicare Part D prescription drug costs - and Medicare Part A or Medicare Part B costs?
Yes. The Medicare Part D Extra Help program is available to help people with limited financial resources pay for their monthly premiums and drug costs. The Extra Help or Low-Income Subsidy (LIS) program is based on a Medicare beneficiary’s income and assets (or financial resources). Most people who qualify for full-extra help will pay no premiums, no deductibles, and no more than a low-fixed cost for each prescription (with this amount changing each year). For more information, please contact your state Medicaid office. Medicare Savings Programs are also available and, depending on your finances, may help pay Medicare Part A and/or Medicare Part B premiums, and maybe some Medicare Part B costs.
No. Medicare Part D coverage will vary plan-to-plan and not all Medicare plans are available in all areas of the country. Remember: Medicare Part D and Medicare Advantage plans are offered in specific Service Areas, such as multiple-states, counties, ZIP code areas, or parts of a highly-populated city such as New York or Los Angeles. This means: If you live in Saint Johns County, Florida, you will not have the same selection of Medicare plans as your friends who live in Orange County, California. Our Q1Medicare.com tools are designed to provide people with an overview of all Medicare plan options in their area or region. For more information on Medicare prescription drug coverage, please call Medicare at 1-800-633-4227.
Question: When can I enroll into a Medicare Part D plan?
Your Initial Enrollment Period - If you are new to Medicare, you have an Initial Enrollment Period (IEP) that is a seven (7) month window beginning three (3) months before your month of eligibility, plus the month of eligibility, and ends three (3) months after your month of eligibility. If you enroll in the three months prior to your month of Medicare eligibility, your effective date (when your plan coverage begins) is the 1st day of your month of Medicare eligibility. If you enroll into a Medicare Part D plan during your month of eligibility (such as when you turn 65) or during the three months following the month of Medicare eligibility, your Medicare Part D plan will be effective on the 1st day of the month following receipt of your plan enrollment.
The annual Open Enrollment Period - If you are already eligible for Medicare, you can change Medicare plans during the Annual Enrollment Period (AEP). The Annual Enrollment Period starts each year on October 15th and continues through December 7th with your Medicare Part D plan becoming effective on January 1st of the new plan year. This time period can also be called the annual Open Enrollment Period -- which is still referred to as "AEP".
Special Enrollment Periods - If you are outside of your IEP or AEP, then you will need to use a Special Enrollment Period (SEP) to change Medicare Part D or Medicare Advantage plans. An SEP may be granted when you move outside of your plan's Service Area (move to another state) or move into an assisted living facility or when you qualify for Extra Help. If you are entitled to an SEP, your Medicare Part D plan will become effective on 1st day of the month following the receipt of your enrollment. See our Special Enrollment Period FAQ for more details and examples of SEPs.
Question: Can you join a Medicare drug plan even though you have outstanding health issues?
Yes. There are no medical limitations to joining a Medicare Part D plan and since 2021, there are no medical limitations when enrolling in a Medicare Advantage plan that provides prescription drug coverage (MAPD). From 2006 to 2020, Medicare Advantage plans required that the Member did do not suffer from End Stage Renal Disease (ESRD) or (kidney failure).
You can choose and join any Medicare drug plan that works for you and is available in your area.
Question: How much will I pay per month for a drug plan?
You will have to pay a monthly premium like you would for other insurance and premiums can range to $0 (for a MAPD plan) up to over $100 per month. If you qualify for the Medicare Part D financial Extra Help program (or Low-Income Subsidy) and enroll in a Medicare Part D plan that meets your state's $0 low-income subsidy benchmark your monthly premium will be $0.
All drug plans must provide coverage that is at least as good as standard Medicare prescription drug coverage. Some plans might offer more coverage and additional drugs for higher monthly premiums.
Question: Am I required to join a Medicare Part D plan?
No. The Medicare Part D program is voluntary and you are not required to enroll into a Medicare Part D plan when you first become eligible for Medicare. However, if you do not have some other form of creditable prescription drug coverage and then later decide to join a Part D plan (PDP or MAPD) you may incur a permanent late-enrollment penalty that you will pay in addition to your monthly plan premiums.
Question: If I don't join a drug plan when I am first eligible, how is the Late-Enrollment Penalty calculated?
Late-Enrollment Penalties are assessed when you eligible for Medicare Part D coverage, but are without some form of creditable drug coverage for more than 63 days. You can learn more in our late-enrollment premium penalty FAQs. Late-enrollment penalties are permanent and can change (increase) year-to-year. You will pay 1% of the national base Medicare Part D premium (about $33) for every month that you were without some creditable prescription drug coverage before you enrolled in a Medicare Part D plan. So, if you were eligible for Medicare when you were 65 and now you are 70, you would pay 60 months worth of penalty (5 years * 12) or about 60% of the annual base premium (so around $33 * .6 = $20 per month in addition to your monthly Part D plan premium).
Question: Is there financial assistance to help me pay my Medicare Part D prescription drug costs - and Medicare Part A or Medicare Part B costs?
Yes. The Medicare Part D Extra Help program is available to help people with limited financial resources pay for their monthly premiums and drug costs. The Extra Help or Low-Income Subsidy (LIS) program is based on a Medicare beneficiary’s income and assets (or financial resources). Most people who qualify for full-extra help will pay no premiums, no deductibles, and no more than a low-fixed cost for each prescription (with this amount changing each year). For more information, please contact your state Medicaid office. Medicare Savings Programs are also available and, depending on your finances, may help pay Medicare Part A and/or Medicare Part B premiums, and maybe some Medicare Part B costs.
Browse FAQ Categories
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
