2021 State Low-Income Subsidy Benchmark Premium Amounts - with a comparison of benchmark changes since 2006
See 2022 Benchmark figures at: 2022 Low-Income Subsidy Premium Amounts - includes 2021 - 2006 for comparison. (Q1News.com/886).
The Centers for Medicare and Medicaid Services (CMS) released the 2021 low-income premium subsidy
amounts (or Benchmark premiums) for Medicare Part D plans on July 29, 2020, and in 2021,
only four (4) regions will lower their Medicare Part D Low-Income Subsidy (LIS)
benchmark values and thirty (30) regions will increase
their benchmark premium.
Here are a few state highlights of the 2021 LIS benchmarks:
- Alaska
will see the largest benchmark decrease with a 2021 LIS subsidy of
$29.77
as compared to
$31.36 in 2020.
Ohio
had the largest benchmark decrease last year.
- Hawaii
will have the largest benchmark increase with a 2021 LIS benchmark
of $31.12
as compared to
$25.21
in 2020.
Arkansas
had the largest benchmark increase in 2020.
- New York
will have the highest 2021 benchmark premium of all CMS PDP
regions at $42.27.
Last year,
Wisconsin
had the highest benchmark premium at $39.91.
- Texas continues to have the lowest benchmark premium at $22.48. Texas had the lowest 2020 benchmark at $20.78.
What is the LIS Benchmark Premium?
The benchmark premium is the maximum* monthly Medicare Part D plan premium that will be paid by CMS for persons qualifying for the low-income subsidy (LIS) or the Medicare Part D "Extra Help" program.
For example, if you qualify for full Extra Help benefits and live in a state with a benchmark premium of $25, the Medicare Part D Extra Help program will pay for the premium of a "Basic" Medicare Part D plan up to this premium level (or slightly above*) and you will have a $0 monthly premium for your drug coverage. If you qualify for partial Extra Help, your monthly premium will not be $0, but your premium will be reduced.
What happens when someone joins a Medicare plan that has a premium higher than the benchmark?
If a person receiving the low-income subsidy enrolls in a Medicare Part D plan that has a premium higher than their state's benchmark premium, the beneficiary is responsible for paying the difference in premiums - unless the difference between the benchmark premium and the plan premium are relatively small (please see the explanation of the de minimis premium policy below*).
In addition, if the full-LIS person enrolls in a low-premium Medicare Part D plan with "enhanced" features, they may also pay a partial premium, even when the plan premium is below the benchmark since the plan is not considered "basic".
Do benchmark premiums change over time?
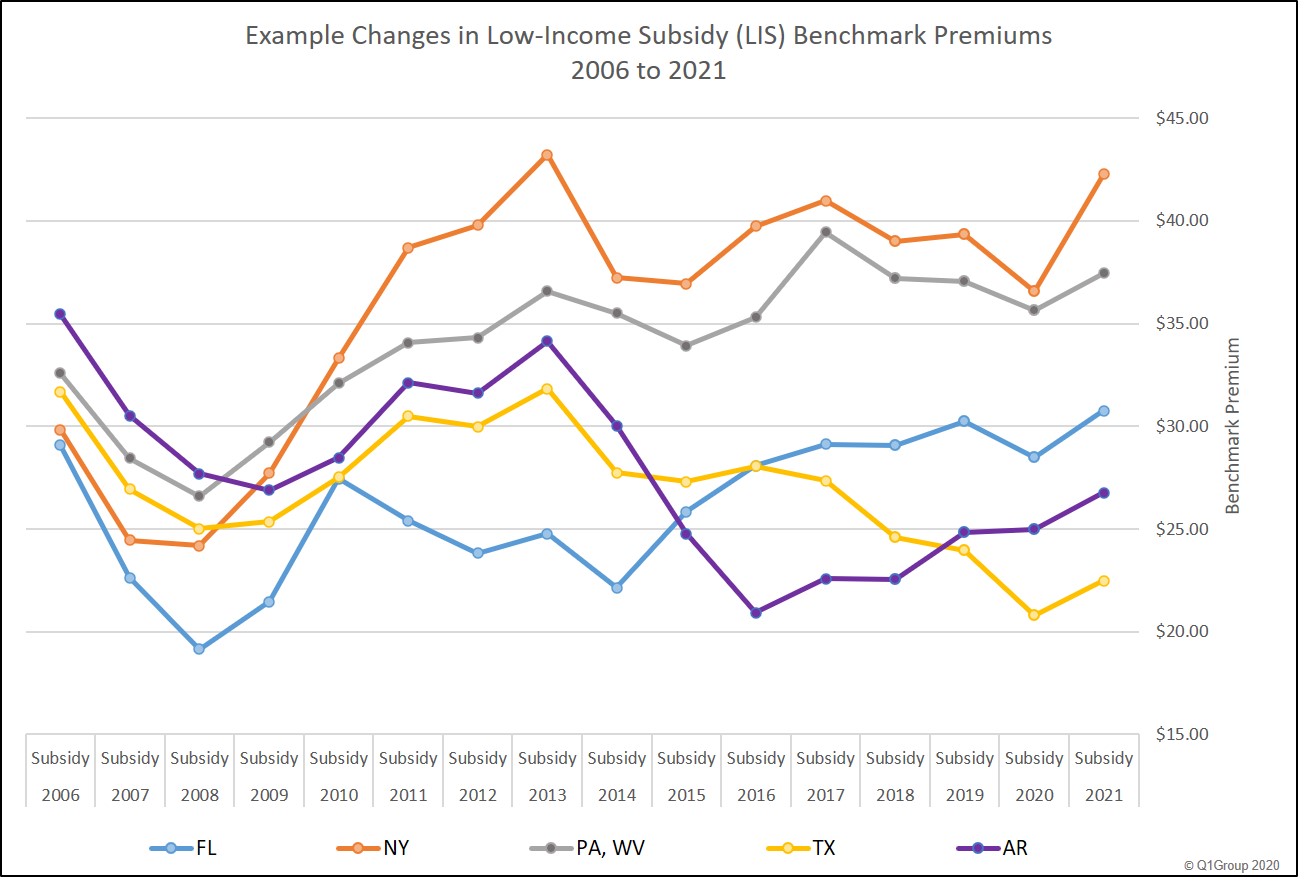
Yes. State LIS benchmark premiums usually change every year and annual decreases (or increases) in Benchmark Premiums may provide an indication that the state will offer Medicare Part D beneficiaries more (or fewer) stand-alone Medicare Part D plans qualifying for the $0 LIS Medicare Part D premium.
As reference, the following chart shows how the annual Medicare Part D LIS Benchmark premiums in a few example states have fluctuated since 2006. The example states were chosen due to their relatively large population of seniors or Medicare beneficiaries.
How many Medicare Part D plans are offered each year that qualify for the $0 premium?
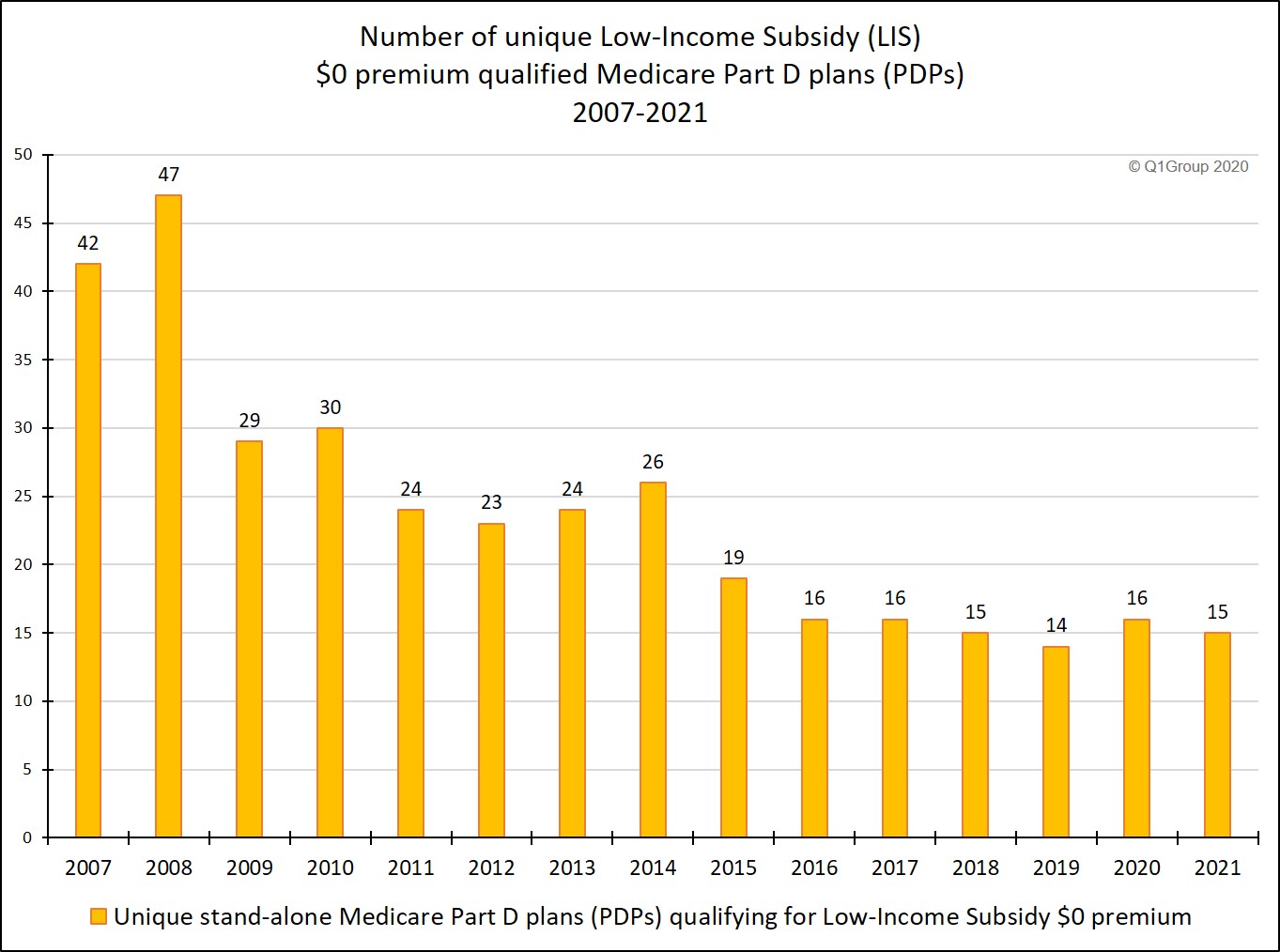
The number of stand-alone Medicare Part D plans qualifying for the $0 LIS premium changes each year, but the general trend is that the number of unique Part D drug plans has begun to level out over the past years as shown by this chart displaying qualifying plans from 2006 through 2020 (2021 Part D plan information will be included when released on October 1st).
*Note: Under the CMS de minimis premium policy, "Part D plans are required to charge full-premium subsidy eligible beneficiaries a monthly Part D beneficiary premium equal to the applicable low-income premium subsidy amount, if the plan’s beneficiary premium for basic prescription drug coverage exceeds the low-income premium subsidy amount by $2 or less."
"Under the Affordable Care Act (ACA) §3303(a), a prescription drug plan (PDP) or Medicare Advantage plan with prescription drug coverage (MA-PD) may volunteer to waive the portion of the monthly adjusted basic beneficiary premium that is a de minimis amount above the low-income subsidy (LIS) benchmark for a subsidy eligible individual. The law prohibits CMS from reassigning LIS members from plans who volunteered to waive the de minimis amount. The de minimis amount for 2021 will be $2. The de minimis amount for 2021 for a plan participating in the Part D Payment Modernization Model will also be $2."
As an example of the de minimis premium policy, in 2020 North Carolina had a benchmark premium of $26.36 and 3 of the 9 Medicare Part D plans qualifying for the full-LIS $0 premium had monthly premiums higher than the benchmark – but still within the “de minimis” range".
**Note: The 2009 low-income benchmark premium amount calculated for region 29 is $19.68. The low-income premium subsidy amount of $20.20 is the lowest monthly beneficiary premium for a PDP that offers basic coverage in region 29. Section 1860D-14(b)(3) of the Social Security Act states that the low-income premium subsidy amount is the greater of the lowest monthly beneficiary premium for a PDP that offers basic coverage and the low-income benchmark premium amount.
The number of stand-alone Medicare Part D plans qualifying for the $0 LIS premium changes each year, but the general trend is that the number of unique Part D drug plans has begun to level out over the past years as shown by this chart displaying qualifying plans from 2006 through 2020 (2021 Part D plan information will be included when released on October 1st).

*Note: Under the CMS de minimis premium policy, "Part D plans are required to charge full-premium subsidy eligible beneficiaries a monthly Part D beneficiary premium equal to the applicable low-income premium subsidy amount, if the plan’s beneficiary premium for basic prescription drug coverage exceeds the low-income premium subsidy amount by $2 or less."
"Under the Affordable Care Act (ACA) §3303(a), a prescription drug plan (PDP) or Medicare Advantage plan with prescription drug coverage (MA-PD) may volunteer to waive the portion of the monthly adjusted basic beneficiary premium that is a de minimis amount above the low-income subsidy (LIS) benchmark for a subsidy eligible individual. The law prohibits CMS from reassigning LIS members from plans who volunteered to waive the de minimis amount. The de minimis amount for 2021 will be $2. The de minimis amount for 2021 for a plan participating in the Part D Payment Modernization Model will also be $2."
As an example of the de minimis premium policy, in 2020 North Carolina had a benchmark premium of $26.36 and 3 of the 9 Medicare Part D plans qualifying for the full-LIS $0 premium had monthly premiums higher than the benchmark – but still within the “de minimis” range".
**Note: The 2009 low-income benchmark premium amount calculated for region 29 is $19.68. The low-income premium subsidy amount of $20.20 is the lowest monthly beneficiary premium for a PDP that offers basic coverage in region 29. Section 1860D-14(b)(3) of the Social Security Act states that the low-income premium subsidy amount is the greater of the lowest monthly beneficiary premium for a PDP that offers basic coverage and the low-income benchmark premium amount.
News Categories
Pets are Family Too!
Use your drug discount card to save on medications for the entire family ‐ including your pets.
- No enrollment fee and no limits on usage
- Everyone in your household can use the same card, including your pets
Your drug discount card is available to you at no cost.
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
